Newsletter 2021
Newsletter July 2021: Major changes and messages in the 2021 Ressuscitation guidelines
Enrique Jesus Carrero Cardenal. Department of Anaesthesiology, Hospital Clínic, University of Barcelona.
ecarrero@clinic.cat
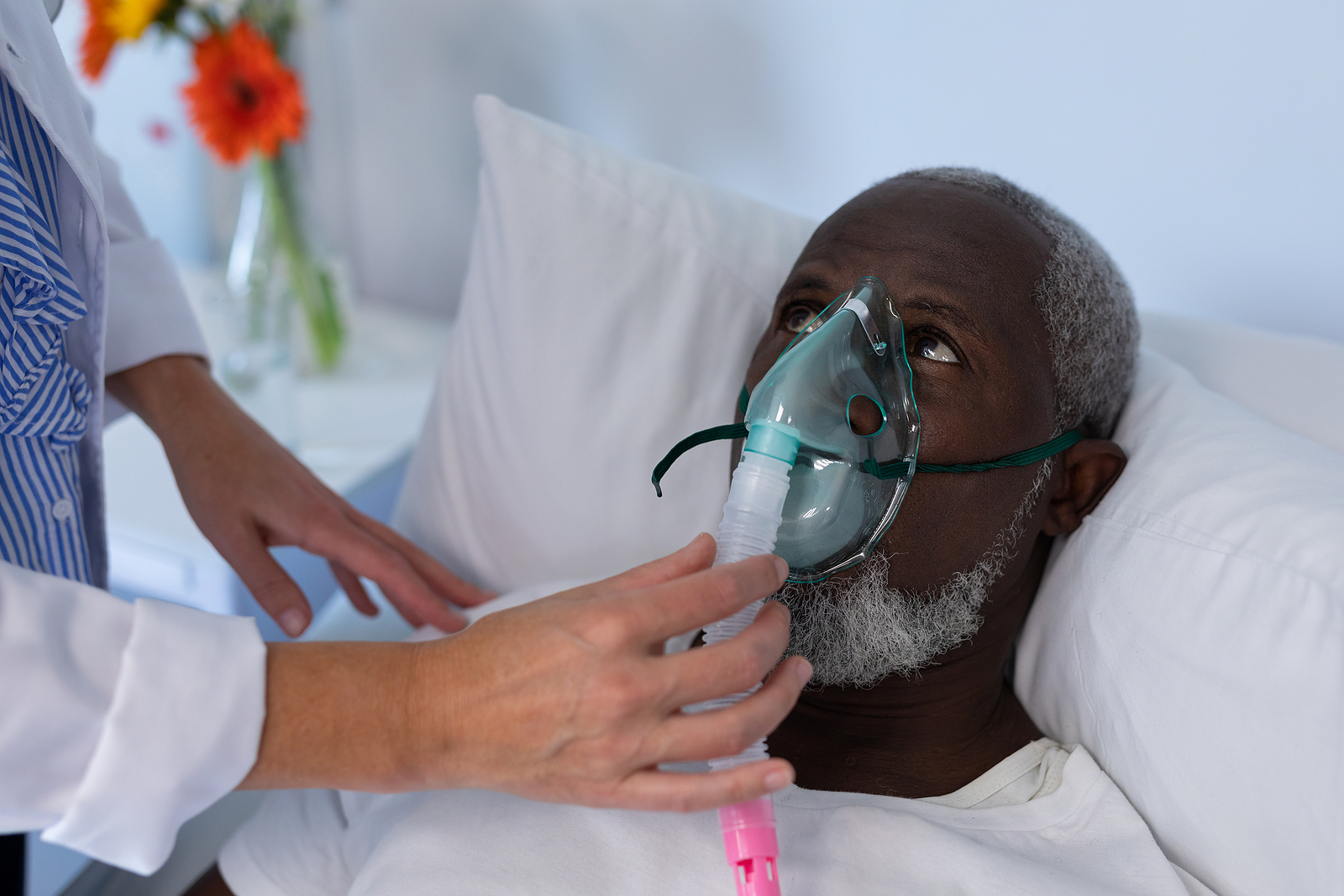
The European Resuscitation Council (ERC) Guidelines are reviewed and published every 5 years. However, due to the pandemic status, the ERC Council decided to postpone the ERC Guidelines 2020 publication until 2021. In 2020, the ERC published what was then a priority: the Guidelines for Covid-19 patients in cardiac arrest (CA).1 On 25-26 March, the Resuscitation ERC guidelines 2021 conference took place virtually from Antwerp, Belgium. The main objective was the dissemination of the new 2021 guidelines. The recorded sessions are available to Cosy ERC members (https://cosy.erc.edu) on the website: https://www.resuscitation.eu/congress-app.html#/program. This article aims to summarise the main changes introduced and highlight the messages emphasized in the presentation of the new ERC 2021 guidelines.
There are no major changes in the 2021 Guidelines compared to the 2015 Guidelines, but there are concepts and messages that are worth a mention. A notable aspect of the new Guideline is the improved presentation format. In the different sections, infographic summaries of the key messages have been added to the different sections, as well as action algorithms and explanatory tables. The executive summary article2 and the articles corresponding to the 11 sections (Epidemiology of CA in Europe, Systems Saving Lives, Basic Life Support (BLS), Adult Advanced Life Support (ALS), CA in Special Circumstances, Post-Resuscitation Care, Newborn resuscitation and Support of Transition of Infant at Birth, Paediatric Life Support (PLS), Education for Resuscitation, Ethics of Resuscitation and End-of-Life Decisions) are already published3-10 downloadable at cprguidelines.eu. The chapter Newborn and paediatric resuscitation will not be covered in this article.
The Epidemiology section recommends the recording of data and information on cardiopulmonary resuscitation (CPR) according to the Utstein methodology: incidence, survival, neurological prognosis etc.
The importance of continuing to develop and apply Systems Saving Lives as a means of involving the wider society in the initial care of the CPR patient is emphasized. These systems include the chain of survival, monitoring the correct execution of chest compressions, the use of social media, the use of smartphone applications (location of AEDs or volunteers) and cognitive aids, campaigns such as the European Restart a Heart Day, World Restart a Heart or Kids Saves Lives, the importance of regularising the use of early warning systems (EWS=early warning system), rapid response systems (RRS=rapid response system), medical emergency teams (MET=medical emergency teams), CA reference centres or the essential role of the dispatcher.
The inclusion of CPR training programmes in schools at an early age (<12 years) has been shown to improve children’s understanding when training programmes are applied at older ages. The message to spread is “saving a life is a child’s play”. Children have the capacity to raise awareness of CPR among their family members. Four hours of teacher training is considered sufficient. Quick teaching schemes are recommended: “Check-call-compress”. New technologies such as apps, games, or virtual reality and low-cost manikins are considered useful tools for teaching CPR in schools.
The 2021 Guidelines on BLS and ALS emphasise recognition of premonitory signs of CPR and prevention measures. The Guidelines highlight the importance of integrating CPR decisions into overall early emergency treatment plans, smartphones as systems for alerting 112 and receiving feedback during CPR, and national databases for locating AEDs.
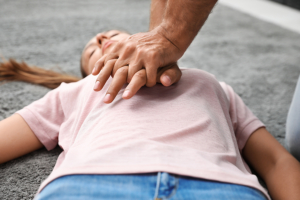
The 5 key messages in BLS are: recognise CA and start CPR, alert emergency medical services, perform chest compressions, use the AED and learn CPR for the majority of the population. The new Guidelines set out a schematic BLS algorithm and an algorithm with detailed instructions for each step to be followed. The sequence of action is unchanged from 2015. The Guidelines emphasize starting CPR on an unconscious victim who is not breathing normally. If there is only one rescuer, it is a priority to start CPR and immediately call 112 with a hands-free mobile phone. It is not recommended to leave the victim to fetch an AED unless the AED is insight. The 112 telephone assistance will indicate to perform chest compressions only for lay rescuers and if the victim is a child will also help with ventilation. Trained rescuers will perform the cadence 30 compressions 2 ventilations. Remember not to stop compressions while placing the AED. There is no change in the systematic use and operation of the AED. One patch at the level of the sternum and the other in the axillary midline below the axilla and above the last rib. Resume compressions if no shock is advised and does not stop compressions until the victim shows signs of life after an experienced professional arrival or the rescuer is exhausted. A lateral safety position is indicated for the unconscious victim who regains breathing but a continuous reassessment of breathing is mandatory.
Early detection of CA, rapid initiation of compressions, high-quality chest compressions (correct hand position “centre of chest = lower half of sternum”, compression rate 100-120 cpm, depth 5-6cm, complete chest release), minimising compression interruption times (<5 s) and early defibrillation continue to be priority measures to improve the prognosis of the CA patient. It is important to remember that for every minute of delay in CPR, survival decreases by 10%. Public access to the AED improves the likelihood of survival and neurological outcome of CA patients.
Compressions can be performed over an article of clothing that allows the chest anatomy to be identified (e.g. a T-shirt). Emphasis is placed on performing chest compressions on a firm surface whenever possible. Throwing the patient to the floor is not recommended because of the loss of time and the possibility of injury. There is no evidence of increased survival associated with the use of feedback devices during CPR.
The recommended energy for the first shock (biphasic defibrillator) is 150J. If the first shock is ineffective, it is recommended to increase the energy (200 J manual defibrillator). In case of refractory ventricular fibrillation, check the correct placement of paddles or pads, especially the paddle or pad at the level of the left mid-axillary line. There are no studies that demonstrate whether anterolateral or anteroposterior paddles or patches are better than the other. In monitored witnessed CA (cath lab, ICU etc) 3 shocks may be given in a row. In these cases amiodarone, 300 mg iv should be administered immediately after the three consecutive defibrillations, followed by 2 min cycles of CPR and defibrillation if the shockable rhythm persists. Adrenaline 1mg and amiodarone 150 mg after the fifth defibrillation and adrenaline every 4 min. For fine fibrillation that may appear to be asystole, the 2021 Guidelines recommend defibrillation. Dual segmental defibrillators have not shown any benefit.
Regarding airway management during CPR, it is recommended to start with basic techniques and progress gradually according to the skills of each rescuer. Supraglottic devices are easier to place, interrupt chest compressions for less time and there is no significant difference in functional prognosis compared to orotracheal intubation. Agonal breathing indicates CPR. In case of convulsions, as soon as the victim stops convulsing, if not breathing, CPR should be initiated. To improve the effectiveness of ventilation, two resuscitators are recommended for manual ventilation. The cadence of 30 compressions 2 ventilations is maintained. Tracheal intubation should only be attempted by rescuers with a high success rate in this technique (> 95% in a maximum of two intubation attempts). There is no difference in intubation success between laryngoscopes and video laryngoscopes, high FiO2 is recommended. In the case of CPR with a laryngeal mask (except inpatient Covid-19) or orotracheal tube, the recommendation of not stopping compressions and ventilating at a frequency of 10x’ is maintained. The importance of using capnography as the most reliable method to confirm tracheal intubation, as a marker of CPR quality or as an indicator of recovery of spontaneous circulation (ROSC) is emphasised. Routine cricoid pressure (Sellick manoeuvre) during intubation is not recommended.
Intravenous or intraosseous access for drug administration is indifferent, the important thing is to reduce cannulation time. CPR drugs are unchanged. Adrenaline should be given as soon as possible in non-shockable rhythms and adrenaline should be given after the third defibrillation in shockable rhythms, then every 3-5 min. Amiodarone is unchanged. Lidocaine is acceptable as an alternative if amiodarone is not available or according to the local protocols of each centre. Administration of thrombolytics if pulmonary embolism is suspected increases CPR time to 60-90 min. Routine administration of bicarbonate, atropine or fluids is still not recommended. The tachyarrhythmia algorithm has been modified to simplify it due to the difficulty in assessing QRS width at high frequencies. Procainamide 10-15 mg Kg-1 mg replaces amiodarone 300 mg in stable regular tachycardias where neither vagal manoeuvres nor adenosine (6,12 and 18mg) have been effective and are wide QRS complex. The 2021 Guidelines recommend cardioversion of unstable atrial fibrillation with maximal energy and not stepwise.
The 2021 Guidelines emphasise prioritising the recognition and management of reversible causes of CA due to Special Circumstances and the increasing utility of e-CPR. They recommend applying ABCDE algorithms + the SVA algorithm. Chest compressions should not delay treatment of the cause. The recommended treatments for electrolyte disturbances, sepsis, coronary thrombosis, accidental hypothermia and avalanche rescue are maintained. Prognosis after rewarming of hypothermic patients follows more specific assessment scales (HOPE scale; ICE scale). In avalanche rescue, priority is given to ventilation, as hypoxia is considered the most likely cause of CA. Recommendations for CA in the haemodynamic ward and in dialysis units have been added. In the management of hyperkalaemia, the efficacy of treatments is preserved, the risk to patient safety is addressed (e.g. risk of hypoglycaemia associated with insulin administration even at 5U doses). It is recommended that prior blood glucose (<7mmol.L-1, <125 mg.dL-1) be assessed as a predictor of hypoglycaemia risk when administering insulin. Also consider the options of new potassium binders, haemodialysis or e-CPR. The Guidelines remind us that below 30ºC adrenaline or defibrillation have no effect and that below 28ºC or 20ºC CPR can be interrupted for short intermittent periods of 5 min (complex transport…). Remember that ETCO2 is not an indicator of CPR efficacy in pulmonary embolism. Two changes in the 2021 Guidelines regarding coronary thrombosis: 1.- it has been included in the section on special circumstances and 2.- the importance of prevention, detection and treatment. If ROSC: fibrinolysis-PCI; if not ROSC: e-CPR. In post-cardiac surgery CA do not use adrenaline 1mg, use 300 mcg (avoids the risk of bleeding or suture dehiscence). In many special circumstances of CPR, prolonging CPR time should be considered and personal protective equipment should not be forgotten as a preventive measure in the event of certain exposures. In single-rescuer CPR for drowning (respiratory cause), give 5 rescue breaths, call 112 and, if no mobile phone is available, perform 1min of CPR before abandoning the victim.
The main changes in Post-resuscitation Care include aspects of general intensive care management such as nutrition, stress ulcer prophylaxis and avoidance of routine use of muscle relaxants. Treatment of seizures (levetiracetam or valproic associated with sedation) is better detailed, including modifications in the prognostic algorithm for patients recovered after CPR (unconsciousness without sedation with motor response ≤3 without confounding factors indicates a poor prognosis. Assessment at 72 hours and presence of 2 or more criteria: absence of pupillary reflexes with pupillometer or corneal reflexes, absence of bilateral N2 or SSEP waves, malignant EEG suppressions or burst suppressions >24h, neuro-specific enolase (NSE) >60 mcg/L at 48h or 72h or progressive increase in levels on days 1, 2nd and 3rd days, myoclonic status <72h, diffuse anoxic oedema MRI or CT). Greater emphasis is placed on functional assessments of physical and non-physical impairments prior to discharge, at follow-up and during long-term rehabilitation. Recommendation on target temperature management (TTM) after CPR awaits future results of randomised controlled studies. Prevention and treatment of hyperthermia are essential.
With regard to the essential concepts in education, it is enacted that the teaching of CPR should be universal, with the aim that any citizen should have the basic skills to save a life. The message that basic CPR techniques are easy to learn and teach is reinforced. Healthcare workers should be trained in ALS and maintain their certification. Simulation and teaching of non-technical skills, the use of cognitive aids and the application of debriefing are encouraged.
There is no evidence of the ideal teaching method for learning non-technical skills. E-learning access as blended learning is useful as long as it is ensured that the information posted is correct. Techniques such as virtual reality or gamification help to increase self-confidence. Simulation allows experimentation in learning technical and non-technical skills, leadership skills, etc. Different simulation modalities from in situ to high-quality simulation are valid alternatives. The teaching of BLS needs to be optimised with tailored programmes, technology-enhanced learning and feedback devices, short refresher courses in competencies and yearly refresher courses, and teacher development through courses for instructors and educators.
Finally, in the Ethics section, essential concepts include a) advance care plans: helping patients and their families achieve the outcomes that are important to them. Enable physicians and patients to participate in shared decision-making. Integrate decisions not to initiate CPR into the emergency care treatment plan; b) educate patients and the public on what resuscitation and outcomes after resuscitation entail and on their role in helping physicians know what outcomes are important to them; c) educate healthcare professionals on the importance of advance care planning, which involves shared decision making, how to communicate effectively with patients and their families when discussing advance care plans; d) when to start and stop CPR using predefined criteria for stopping or withholding CPR, not basing decisions on isolated clinical signs or markers of poor prognosis, and documenting the reasons for resuscitation decisions; e) research: involve patients and the public during the design, conduct and interpretation of the research, respect the dignity and privacy of research participants, follow national guidelines for conducting research in an emergency where people lack capacity.
The importance of communication strategies and interventions to support discussions with patients and their families is recognised, as well as the need for support to be offered to family members witnessing resuscitation attempts. There is a need for health systems to monitor outcomes following CPR to help reduce variability in patient outcomes.
References
- Nolan JP, Monsieurs KG, Bossaert L, et al.. Resuscitation 2020: 153:45-55.
- G.D. Perkins, Graesner JT , Semeraro F, et al. Resuscitation 2021; 161:1-60.
- JT Gra¨sner, J Herlitz, IBM. Tjelmeland, et al., Resuscitation 2021; 161:61-79.
- F Semeraro, , R Greif , BW Böttiger, et al., Resuscitation 2021; 161:80-97
- J Soar, BW. Böttiger, P Carli, et al. Resuscitation 2021; 161:115-151.
- C Lott, A Truhla´r, A Alfonzo, et al., Resuscitation 2021; 161:152-219.
- JP Nolan, C Sandroni , BW. Böttiger, et al. Resuscitation 2021; 161:220-269.
- P Van de Voorde, N M. Turner , J Djakow et al.
- R Greif, A Lockey, J Breckwoldt, et al., Resuscitation 2021; 161:388-407.
- SD. Mentzelopoulos, K Couper, P Van de Voorde, et al. s, Resuscitation 2021; 61:408-432.
Read our Monthly newsletter.
Read More of our special newsletter covering our virtual congress 2020.
Visit our COVID-19 Resource Hub for other news and resources.