Newsletter 2022
Newsletter May 2022: Three-dimensional Printing in Anaesthesia – Do It Yourself
Ruth Shaylor, MD
Ruth.shaylor@gmail.com
To be featured in the Euroanaesthesia Milan Session 11P1 Airway management future: ingenious ideas! – on Saturday 4 June, 1630H, Room Amber 3
It has been impossible to avoid three-dimensional (3D) printing over the last two years whether it’s a 3D-printed ventilator, a 3D-printed mask, or even the 3D-printed ear protectors that we all use. In addition, 3D printing, and virtual reality (VR) have entered clinical practice in recent years, and are increasingly being used in various specialities, such as maxillofacial and orthopaedic surgery. Their main uses are preoperative planning and the development of personalised implants. 12
Computer-assisted design (CAD) programs can be used to make anatomically correct models from a patient’s computerised tomography (CT) or magnetic resonance images (MRI). Once this modelling is completed, it can be printed using a 3D printer or converted into a VR reconstruction used with commercially available headsets (figure 1), providing anatomically correct patient-specific models. Whilst these technologies have demonstrated benefits in education and training current clinical use is limited to case descriptions of successful management of particularly challenging patients. 34
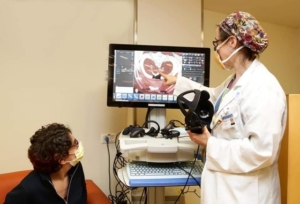
Figure 1: Discussing a VR model with a colleague
In 2019, the anaesthesia department at Tel Aviv Medical Center (TLVMC) began to implement 3D airway modelling in the routine preoperative assessment of all patients presenting with a suspected complex or potentially challenging airway. Patients are referred for preoperative modelling either by the surgical service or the preoperative anaesthesia clinic.
For printed models, the treating anaesthesiologist will select their preferred airway equipment (e.g., double-lumen tube, endotracheal tube, bronchial blocker), and test it on the model. The anaesthesiologist is allowed to try as many airway solutions as they want before choosing the one they find most suitable for the case.
When VR reconstructions are performed, we use the SurgicalTheatre™ volume rendering software (SurgicalTheatre, Cleveland, Ohio, United States). This system reconstructs digital 3D models using DICOM images by automatic identification of different tissue densities according to the grey value of each pixel. These 3D reconstructions are viewed on commercially available VR headsets (Oculus, Facebook, California, USA) (Figure 1). This allows the practitioner to navigate through the structures and to visualise their different anatomical relationships.
In cases of anterior mediastinal masses, 3D reconstructions are discussed with the cardiothoracic surgery service to consider the need for extracorporeal membrane oxygenation (ECMO) as part of the anaesthetic plan.
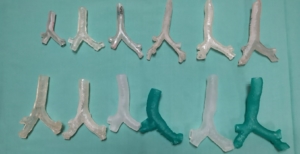
Figure 2: a selection of printed models
To date we have used 3D modelling in twenty patients, of these 15 models were printed including 12 children requiring one-lung ventilation (Figure 2). Five patients had VR reconstructions including 3 with mediastinal masses. One patient had a 3D printed model and VR reconstruction. There were two cases (10%) where the model plan did not correlate with the final airway plan and one case where a model could not be made at all. This was due to poor original imaging. For the remaining 17 cases, the plan devised on the model was also the final airway plan. There were no anaesthetic complications.
Aside from image quality, there are other challenges associated with setting up a clinical 3D service. For example, which CAD programs and which printers to use. Whilst this is currently a fairly unregulated market this is likely to change in the next few years. The FDA has recently finished a public consultation in the area. Obviously, regulation is important but it will also come with added costs, something that must be factored in for those thinking about using this technology
In this session (see here) we will go over a step-by-step process for making a model, the types of technology involved, and future directions. Most importantly we will see if it is possible to “do it yourself” or whether you need a little help from friends and colleagues.
References
- Jandali D, Barrera JE. y. Curr Opin Otolaryngol Head Neck Surg. 2020;28:246-250. doi:10.1097/MOO.0000000000000638
- Martinez-Marquez D, Mirnajafizadeh A, Carty CP, Stewart RA.. PLoS One. 2018;13(4). doi:10.1371/journal.pone.0195291
- Shaylor R, Verenkin V, Golden E, Matot I.. Eur J Anaesthesiol. 2020;37(6). doi:10.1097/EJA.0000000000001184
- Chao I, Young J, Coles-Black J, Chuen J, Weinberg L, Rachbuch C. T Anaesthesia. 2017;72:641. doi:10.1111/ANAE.13812
[maxbutton id=”1″ url=”https://www.esaic.org/newsletter/” text=”Read the Newsletter” ]










