Congress Newsletter 2022
The big five in resuscitation
Session 10S1 held on Sunday 5 June, 1100-1200H, Space 3
This session is available OnDemand on the Euroanaesthesia platform
Sunday afternoon’s sessions included a lively symposium on resuscitation, in which three experts discussed ‘The big five in resuscitation – what really does improve outcome in 2022’?
The first talk provided updates on three of these five topics: lay resuscitation. telephone CPR and recognition of cardiac arrest, and was given by Professor Federico Semeraro, Consultant in Anaesthesia and Intensive Care, Maggiore Hospital Bologna Italy and Chair-Elect of the European Resuscitation Council (ERC).
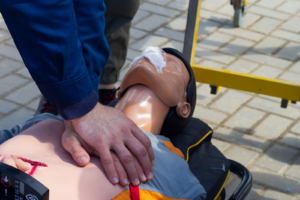
He discussed how early cardiopulmonary resuscitation (CPR) and defibrillation can double survival after out-of-hospital cardiac arrest (OHCA). “Improving the first links of the chain of survival is of paramount importance to save more lives,” he explained. “Lay response is key to achieve this goal and can be supported by different actors at a system level through education in recognition and basic life support and telephone CPR provided by emergency services dispatchers.”
He also discussed the latest technology relevant to this area, which is currently being implemented with smartphone apps to alert first responders and explained how in the future the role of technology will be more and more vital, in particular for unwitnessed out-of-hospital cardiac arrest (OHCA) for which survival is currently lower than 1%.
In the second part, first responder systems were specifically addressed by Dr Bibiana Metelmann, of the Department of Anaesthesiology at the Medical University of Greifswald, Germany.
She explained how OHCA depends on a well-functioning chain of survival. “Especially the early start of chest compressions and defibrillation (AED) can improve outcomes,” she explained. “However, bystander-CPR rates in Europe are still low.”
Yet, as a high percentage of the population is trained in resuscitation and is willing to help, the probability is quite high that one of these persons is in close geographical proximity to a cardiac arrest. Therefore, technological solutions to alert these first responders to a cardiac arrest have been invented.
In the new campaign “Systems saving lives” of the European Resuscitation Council, the implementation of first responder systems is one of the 5 top messages. “A systematic review from 2022 came to the conclusion, that these systems were associated with higher rates of bystander-CPR, use of AED before EMS arrival and survival at hospital discharge,” explained Dr Metelmann. “Yet, as first responder systems differ in several aspects and there are still many open research questions, there is a high need for a reporting standard for publications.”
In the final talk, Associate Clinical Professor and Anaesthetist Dr Joyce Yeung of Warwick Medical School, University of Warwick, UK, asked: “does care at a cardiac arrest centre improve outcome after out-of-hospital cardiac arrest?”
She explained there is wide variability in survival among hospitals caring for patients after resuscitation from OHCA. And while OHCA is common, survival outcomes are poor, with substantial regional and international variation, survival from OHCA ranges from 8 to 16%.
Dr Yeung said: “In most countries, post-resuscitation care is not regionalised to specialised hospitals. There is wide variation among hospitals in the availability and type of post-resuscitation care, as well as clinical outcomes. Patients with other time-sensitive emergencies (such as trauma, acute myocardial infarction and stroke) are often triaged to centres which offer speciality services and greater provider experience. Such centralised specialist services may improve the provision of targeted post-resuscitation care and offer similar benefits and improve patient outcomes after cardiac arrest.”
In her talk, she explained what a Cardiac Arrest Centre (CAC) actually consists of and how care at CACs may improve patient outcomes. She examined the evidence behind the International Liaison Committee on Resuscitation (ILCOR) 2019 treatment recommendation which suggests that adult patients with non-traumatic OHCA cardiac arrest be cared for in CACs rather than in non-CACs. This evidence also forms the basis of European Resuscitation Council and European Society of Intensive Care Medicine guidelines. She examined what the published data reveal and where research gaps remain.”
Read More of our special newsletter covering our congress.










